
Vitamin D is an essential nutrient that plays a vital role in maintaining overall health and well-being. It is primarily known for its role in calcium absorption and bone health, but emerging research suggests that it may have a broader impact on various bodily functions, including migraine management.
Several studies have suggested a correlation between low levels of Vitamin D and increased frequency of migraine attacks. A study published in The Journal of Headache and Pain found that participants with chronic migraine attacks had significantly lower Vitamin D levels compared to those without migraine attacks. While the exact mechanisms behind this relationship are still being investigated, researchers believe that Vitamin D deficiency may contribute to the development and persistence of migraine attacks.
Vitamin D plays a crucial role in regulating the immune system, and deficiencies in Vitamin D can lead to chronic inflammation. This chronic inflammation may impact the blood vessels and nerves surrounding the brain, potentially triggering migraine attacks. Vitamin D also plays a role in regulating serotonin production, a neurotransmitter that helps regulate pain and mood. Additionally, low Vitamin D levels have been associated with higher levels of calcitonin gene-related peptide (CGRP), a protein involved in the transmission of pain signals in migraine attacks.
Vitamin D supplementation can be seen as part of a comprehensive approach to migraine prevention and relief. It is not a standalone solution, but rather an additional tool that can be integrated into a holistic management plan. Lifestyle modifications, such as maintaining a regular sleep schedule, managing stress, staying hydrated, and identifying trigger factors, are fundamental aspects of migraine management.
The potential role of Vitamin D in migraine prevention and relief is an exciting area of research. While more studies are needed to fully understand the mechanisms and benefits, current evidence suggests that maintaining adequate Vitamin D levels may have a positive impact on migraine frequency and severity. You can discuss and monitor your Vitamin D levels with a provider at MCHN/Nervana, and when appropriate, integrate Vitamin D supplementation into a comprehensive migraine management plan.
–Alice Wong, NP
https://migrainebuddy.com/the-role-of-vitamin-d-in-migraine-prevention-and-relief
Category Archives: Uncategorized
MIGRAINES TRIGGERED BY SUMMER HEAT

Changes in weather are among the most common triggers reported in patients who have migraine headaches. Shifts in barometric pressure are believed to start an inflammatory cascade which could lead to a migraine episode. However, the exact Patho mechanism is still unclear.
Summer is near, which means warmer weather, dry air, extreme heat and high humidity. These weather conditions may lower migraine threshold. Here are a few tips to help prevent Summer/Heat – Related Migraines:
Hydrate! Hydrate! Hydrate!
Wear protective sunglasses and wide brim hats to keep yourself cool
Stay up to date with daily weather and temperature changes.
Exercise and complete errands in cooler morning or evening hours
Continue to track headache frequency and severity.
By: Jordan Shankle, PA
Idiopathic Intracranial Hypertension

Idiopathic intracranial hypertension (IIH) is a condition that causes pressure inside the skull. It is also called “pseudotumor cerebri.” High pressure around the brain causes headaches and vision loss. Doctors do not know what causes IIH, but it is more common in females and people who have obesity.
The symptoms include:
●Bad headaches – Some people say that the worst pain is right behind their eyes.
●Short periods of vision loss – This can happen in 1 or both eyes. It usually lasts a few seconds, and might happen once in a while or several times a day.
●Dimming of vision
●Trouble seeing things at the edge of your line of sight
●Double vision
●Seeing flashing lights
●Noises inside your head – The noise might sound like rushing water or wind. It often pulses in time with your heartbeat, and can come and go. Doctors call this “tinnitus.”
In rare cases, people with idiopathic intracranial hypertension lose their vision forever.
If you suspect IIH, please make an appointment today with your ophthalmologist, a provider at MCHN/Nervana, or go to the emergency room for sudden/alarming symptoms.
–Alice Wong, NP
SLEEP

Sleep is a fundamental aspect of our life. Adequate amounts of sleep help maintain a healthy brain function and improves overall physical and mental health. While sleep is a vital necessity, almost 50% of the population suffer from various types of sleep disorders. Overtime inadequate amounts of sleep can lead to chronic health conditions including cognitive impairment, increased anxiety and depression and headaches.
The relationship between neurological conditions and sleep disorders is complex, multidimensional, and often bidirectional. Comorbidities of both sleep and neurological disorders often decrease a person’s overall quality of life.
Here are a few helpful sleep hygiene tips:
Maintain a consistent sleep routine/schedule. For example, go to bed and wake up close to the same time daily, even on weekends.
Try mindfulness breathing and relaxation techniques 30 – 45 minutes prior to bedtime.
Take a warm or hot shower prior to bedtime.
Increase physical activity during the day, ie 30 – 45 minutes of exercise. Avoid intense workouts closer to bedtime.
Avoid caffeinated beverages or stimulates late in the day.
Aromatherapy with essential oils.
Try herbal teas. Chamomile and other herbal teas can help relax and sooth the body.
Avoid watching television or excessive screentime on phone or laptops while in bed.
Commit to a well-balanced diet.
Limit Daytime days.
“ The best bridge between despair and hope is a good night’s sleep.”
— E. Joseph Cossman
By: Jordan Shankle, PA
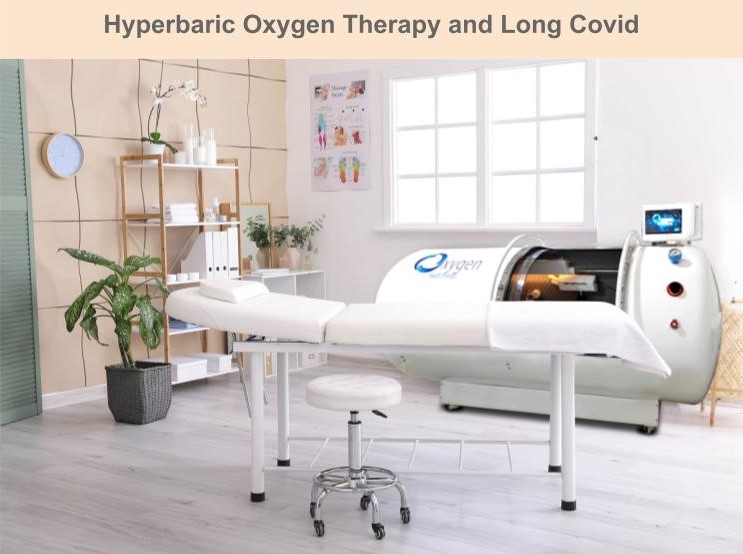
Hyperbaric Oxygen Therapy and Long Covid
Our body’s tissues need oxygen to function. The air we breathe is 21% oxygen.
Hyperbaric oxygen therapy (HBOT) involves breathing 100% (pure) oxygen while in a special space called a hyperbaric chamber. The air pressure inside is raised to a level that is higher than normal air pressure. The increased air pressure in the chamber helps the lungs collect more oxygen. Getting more oxygen to the tissues that need it can help the body heal. HBOT is well known for treating scuba and deep-sea divers affected by the rapid change in pressure around them. HBOT is also used to treat a variety of health problems including anemia, burns, skin infections and wounds.
HBOT is being studied for other conditions, including long COVID-19, where symptoms persist 12 weeks after the initial infection. Common symptoms are fatigue, post-exertional malaise and cognitive dysfunction. The underlying mechanisms are unknown, although several hypotheses exist, with chronic inflammation as a common denominator. In prospective studies, hyperbaric oxygen therapy (HBOT) has been suggested to be effective for the treatment of similar syndromes such as chronic fatigue syndrome and fibromyalgia.
HBOT is thought to provide anti-inflammatory and anti-proinflammatory effects likely to reduce the overexuberant immune response common to COVID-19. Unlike steroids, it exerts these effects without immune suppression. We are pleased to offer HBOT sessions at our Brooklyn location. Please call to inquire about this therapeutic and adjunctive treatment.
–Alice Wong, NP
https://www.fda.gov/consumers/consumer-updates/hyperbaric-oxygen-therapy-get-facts
https://www.uptodate.com/contents/hyperbaric-oxygen-therapy
POLYNEUROPATHY
Polyneuropathy is a term that refers to a generalized process affecting many peripheral nerves, most commonly distal nerves. Clinical symptoms include numbness and tingling, hypesthesia muscle weakness, decreases or increased muscle tone, reduced or diminished reflexes and pain.
The causes for polyneuropathy vary including diabetes mellites, autoimmune disease, toxins, systemic disease, and vitamin deficiency. The role of nutrition regarding the cause and treatment of polyneuropathy has been studied extensively supporting the hypothesis that b vitamins play a crucial role in nerve health; more specifically B12 and B6.
Vitamin b6, is a water- soluble vitamin that is present naturally in foods. It is also available as a supplement. Vitamin b6 deficiency and toxicity has been associated with neurological conditions such as depression, confusion, and neuropathy.
Evaluation of polyneuropathy includes laboratory testing to assess systemic and metabolic causes and assess vitamin levels. Additional testing, ie nerve conduction study or MRI, may be needed to rule out motor neuron involvement.
If you are experiencing these symptoms, schedule a consultation with one of our providers at The Manhattan Center for Headache & Neurology or it’s sister site, Nervana Neurospa.
By: Jordan Shankle, PA
Transverse Myelitis
Transverse myelitis is a rare neurological condition characterized by inflammation of the spinal cord. This inflammation interrupts the signals that the spinal cord nerves send throughout the body, leading to various symptoms such as weakness, numbness, tingling sensations, and in severe cases, paralysis. The onset of transverse myelitis can be sudden, often causing rapid progression of symptoms within hours or days, though it can also develop more gradually over time. While the exact cause of transverse myelitis is often unknown, it is believed to be an autoimmune disorder, where the body’s immune system mistakenly attacks its own tissues. Diagnosis typically involves a thorough medical history, physical examination, and imaging tests such as MRI to assess the extent of spinal cord inflammation.
Treatment for transverse myelitis focuses on managing symptoms and addressing the underlying cause of inflammation. This often involves a combination of corticosteroids to reduce inflammation, pain medications to alleviate discomfort, and physical therapy to help regain strength and mobility. In some cases, other medications to suppress the immune system or intravenous immunoglobulin therapy may be prescribed to modulate the immune response. While many individuals with transverse myelitis experience significant improvement in symptoms with treatment, some may continue to have long-term complications such as chronic pain or mobility limitations. Thus, ongoing medical care and support are essential to optimize quality of life for those affected by this challenging condition.
Beh SC, Greenberg BM, Frohman T, Frohman EM. Transverse myelitis. Neurol Clin. 2013 Feb;31(1):79-138. doi: 10.1016/j.ncl.2012.09.008. PMID: 23186897; PMCID: PMC7132741.
Rodríguez Y, Rojas M, Pacheco Y, Acosta-Ampudia Y, Ramírez-Santana C, Monsalve DM, Gershwin ME, Anaya JM. Guillain-Barré syndrome, transverse myelitis and infectious diseases. Cell Mol Immunol. 2018 Jun;15(6):547-562. doi: 10.1038/cmi.2017.142. Epub 2018 Jan 29. PMID: 29375121; PMCID: PMC6079071.
By: Andrew Chan, PA
VERTIGO

Vertigo is a disruptive sensation of spinning or movement when a person is not actually moving. It is often described as feeling dizzy, lightheaded, or experiencing a spinning sensation. Vertigo can result from various underlying causes, including inner ear problems, such as benign paroxysmal positional vertigo (BPPV), vestibular neuritis, Meniere’s disease, or even more serious conditions like vestibular migraines or acoustic neuromas. The sensation of vertigo can be triggered by sudden head movements, changes in position, or even simply lying down or getting up from bed. While vertigo itself is not typically a serious condition, it can significantly impact daily activities and quality of life, leading to falls, accidents, and anxiety in severe cases.
Diagnosis of vertigo often involves a comprehensive medical history, physical examination, and specialized tests such as the Dix-Hallpike maneuver or electronystagmography to assess inner ear function and rule out other potential causes. Treatment for vertigo depends on the underlying cause and may include vestibular rehabilitation exercises to improve balance and reduce symptoms, medications to alleviate nausea and dizziness, or surgical interventions in rare cases. Lifestyle modifications, such as avoiding sudden head movements or triggers, can also help manage vertigo symptoms effectively. Overall, early diagnosis and appropriate management are crucial in providing relief and improving the quality of life for individuals experiencing vertigo. Schedule a consultation with one of our providers at The Manhattan Center for Headache & Neurology or it’s sister site, Nervana Neurospa.
By: Andrew Chan, PA
Kim JS, Newman-Toker DE, Kerber KA, Jahn K, Bertholon P, Waterston J, Lee H, Bisdorff A, Strupp M. Vascular vertigo and dizziness: Diagnostic criteria. J Vestib Res. 2022;32(3):205-222. doi: 10.3233/VES-210169. PMID: 35367974; PMCID: PMC9249306.
Migraine-Associated Stroke
Migraine is a common headache disorder characterized by symptoms that typically occur over several hours to a few days. Migraine-associated stroke (also known as migrainous infarction or migraine-induced stroke) is an uncommon complication of migraine identified by ischemic stroke on neuroimaging that corresponds to prolonged aura symptoms in a patient with migraine.
The reported incidence of stroke due to migraine (migrainous stroke) ranges from 0.8 to 3.4 per 100,000 per year.
Clinical factors associated with an elevated risk of stroke in patients with migraine include:
-Patients with migraine with aura
-Female patients
-Patients who smoke
-Patients who take estrogen-containing contraception
-Patients age <45 years
Clinical symptoms of migraine-associated stroke are typically similar to previous migraine aura without new or atypical symptoms. However, the previously transient aura symptoms persist for longer duration.
Migrainous infarction occurs in a patient with migraine with aura that is typical of previous attacks except that one or more aura symptoms persists for >60 minutes. Neuroimaging demonstrates ischemic infarction in a relevant area.
Both cerebrovascular events and migraine attacks can present as acute transient neurologic events with similar symptoms. In addition, acute neurologic symptoms that are persistent may also be caused by either migraine or stroke.
For new or alarming symptoms persisting for longer duration, please seek emergency or urgent care. For an evaluation for ongoing care, please make an appointment with one of our caring providers today.
–Alice Wong, NP
https://www.uptodate.com/contents/migraine-associated-stroke-risk-factors-diagnosis-and-prevention
Migraines and Anxiety

Migraines are a type of headache that causes moderate to severe head pain with varying degrees of sensations that differ from person to person. It currently affects 12% of the population in our country. As we gather history and physical evidence from patients, it is shown to be prevalent in those with psychiatric comorbidities. Of these conditions, anxiety was at the top of the list. Why is that? Migraine and anxiety are very closely related due to their similar clinical features, presentation methods, and the episodic nature of their attacks (Kumar et al., 2022). Norton et al. conducted a study in 2004 using structural equation modeling among patients experiencing recurrent headaches; the results of the study concluded that pain-related fear, escape, and avoidance behavior are greatly affected by Anxiety Sensitivity in patients with recurrent headaches (Kumar et al., 2022). In patients with chronic migraine that suffer from repeated migraine attacks, it is also found that there is an alteration in the architecture and function of several regions of the limbic system and also an alteration in the functional connectivity of the hippocampus with other brain regions (Kumar et al., 2022). Not only is this a bidirectional relationship, where one increases the risk of the other, but it has also caused changes in several brain regions. Isn’t that so interesting to know? As providers, this is why it is crucial for us to screen and treat anxiety disorders in patients with migraines effectively.
R. Kumar, S. Asif, A. Bali, D. Gonzalez (2022). The Development and Impact of Anxiety With Migraines: A Narrative Review. Cureus 2022 Jun; 14(6): e26419. Published online 2022 Jun 29. doi: 10.7759/cureus.26419
By: Sheina Roberts, NP
